The Challenge to Embed Telepsychiatry
John Mitchell, BA (Hons), Dip Ed, M Ed Admin, AFAIM Benjamin Mitchell, BA (Psych.), December 1994
Executive Summary
This evaluation study identifies a crucial challenge for the South Australian Mental Health Services (SAMHS) and the South Australian Health Commission (SAHC): how to ensure that the significant successes of the 1994 Telemedicine Pilot Project lead to the embedding of telepsychiatry in the SAMHS and the SAHC.
Background
The evaluation of the Telemedicine Pilot Project was undertaken from June-October 1994.
Telemedicine involves the use of telecommunications technology for the delivery of health care to remote locations and for other purposes such as staff training, administration and patient support. The particular telecommunications technology used in this project provided for the transmission of live, two way videoconferencing, using digital compression. Telepsychiatry is the application of telemedicine in the mental health field.
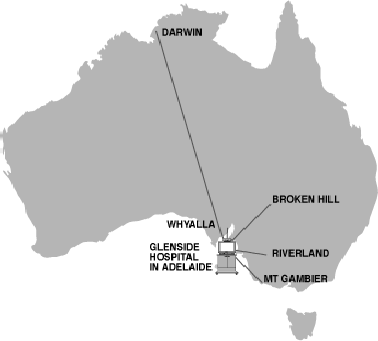
The videoconferencing equipment linked clinicians and other health workers at Glenside Hospital in Adelaide, Berri Hospital, (255km from Adelaide) and Mt Gambier Hospital (400km). Although Whyalla Hospital (400km) was not formally part of this Project, some evaluation of their use of the facilities is recorded in this report. Trial links were also established with Darwin and Broken Hill. The map opposite displays the sites involved with the project.
This evaluation focuses on the ‘non-clinical’ aspects of the pilot such as the types of uses, rate of use, user acceptance, user friendliness, cost effectiveness, productivity gains, technology reliability and effectiveness and the use of the facilities for service delivery and education and training.
An evaluation of clinical aspects of the pilot is being undertaken separately by Dr Michael Baigent, who is comparing interviews of patients by psychiatrists in face to face settings with those interviews involving telecommunication.
The experience of the consultant, John Mitchell from John Mitchell & Associates, is set out in Appendix A.
Objectives and Methodology
The SAMHS received a grant from the Health Commonwealth Network in 1993 to enable it evaluate the use of telecommunications equipment for a number of applications including telepsychiatry, that is, professional psychiatric support for clinical services delivered over a videoconferencing link, mental health team training and development and case management reviews.
The objectives of the project included:
- to design an evaluation process to assess the impact of the telemedicine health system on performance indicators set out below
- to implement and co-ordinate the evaluation process for clinical applications and administration and education
- and to analyse the following performance indicators: technical, economic, usage and acceptance of the system, productivity gains, service delivery and education and training.
The project Brief is set out in more detail in Section One and Appendix B.
The methodology for the evaluation is also discussed in Section One and included a review of the literature (see Section Two and Appendix C), the use of a User Survey (Appendix D), interviews (Appendix E), observations on-site at both Glenside and Berri Hospitals, a Log of Uses (Appendix F) and regular dialogue with the Project Co-ordinator over the five month period.
Major Findings
The major theme of this study is that the SAMHS Pilot Telemedicine Project has achieved much in 1994 but the project is in a fragile state after its first six months of operation. The achievements include:
- the Log of Uses demonstrate that the facilities were used by a wide range of health care related bodies for numerous applications, including clinical consultations, staff training and community health activities (see Section 6 and Appendix F)
- a User Survey completed by 77 users gave resounding support for the medium (4)
- interviews with stakeholders at Glenside, Berri and Mt Gambier revealed strong support among a range of personnel and staff are convinced that the medium is effective for a range of clinical, training and administrative purposes (5)
- the literature review indicates that there are aspects of this pilot, such as the breadth and quality of mental health applications, that are of international significance (2)
- the willingness of the emergency section at Glenside Hospital to use videoconferencing for urgent consultations with the country mental health teams is a significant breakthrough (7)
- a number of patients were able to stay in their country town rather than be transferred to Glenside for an assessment, because of the use of the telemedicine facilities (5,6).
Compared to similar telepsychiatry projects undertaken overseas, the SAMHS project has produced outstanding results in its first year. However, as could be expected in any pilot project, problems and issues have arisen and will need addressing in the near future:
- while many organisations have used the facilities either once or twice, very few have become regular users (4)
- only four psychiatrists used the facilities more than five times, and one more than ten, between May and October and only two general practitioners have been involved (5)
- it is unclear to the outsider as to how much the SAMHS telemedicine equipment is meant to be used by psychiatrists, how much it is to be used by other practitioners in the mental health field and how much it is to be used by other medical fields (5)
- most users have declined the offer of training (4)
- the codec equipment at Berri and Mt Gambier is unreliable and prone to breakdown (3,5)
- legal and ethical problems regarding telepsychiatry need further investigation (5)
- if the handful of significant advocates or users of the telemedicine facilities at each of the three sites was to withdraw from active participation in the project, the project would flounder (7)
- the funds for the project will be almost exhausted by January 1995, and yet the project needs continued strong resourcing to protect the gains of 1994 (7).
Cost effectiveness issues are discussed in Section Six and the following are summary points:
- use of tele-psychiatry will require additional funding, to account not only for the equipment and transmission costs and the necessary administration, but also to account for additional services that could be offered to the many people in country areas presently denied access to mental health care
- whilst on the basis of current client demand, some savings could be made by the SAMHS in terms of the reduction in the number of hospital beds that could be required each year and a reduction in the number of patients transported by ambulance or the police (which could be as high as 50% of annual figures), as a result of assessments conducted using telepsychiatry, telepsychiatry may also uncover presently unmet needs.
In terms of the stages that any innovative technology based project moves through, the telemedicine project is in a normal early stage where it is dominated by “early adopters” who will support a new approach if they can see benefits arising. For the project to survive, it now needs to move to the next stage where more conservative “early majority” users, who like to know that the risks in using the equipment have been removed and who can see concrete benefits arising, become involved. “Early majority” users will only join in if the project is robust, well resourced and likely to succeed. For the “early majority” to provide support, telepsychiatry needs to be embedded as a normal way of providing mental health care in the SAMHS.
It needs to be stressed that most projects involving videoconferencing take at least 2-3 years before usage reaches an optimal level, and the SAMHS equipment has only been operating since 20 April 1994.
In summary, the telepsychiatry network is at a vulnerable stage after its first six months of operation: it needs ongoing funding support, a clear policy framework, improved equipment and maintenance arrangements, vigorous promotion and continued strong management if it is to prosper in its second year.
Major Recommendations
It is recommended that
- The SAMHS, in conjunction with the SAHC, develop a policy framework and appropriate funding for telepsychiatry as an embedded component of rural health services in South Australia. The policy needs to include project objectives for the next 3 years, performance targets for these three years of the network’s operation and a position on legal and ethical matters. (See Section 7)
2. The SAMHS identify funding and develop a budget to ensure that the pilot is adequately resourced in 1995-97, including the ongoing provision of a project manager and support staff and replacement of unreliable codec equipment at Berri and Mt Gambier. (3,7)
3. The emergency section at Glenside Hospital be provided with extra resources to enable it to provide dedicated telepsychiatry support to country based mental health teams. (7)
4. Use of the telepsychiatry network for the delivery of a wide range of mental health and other health services and for education and training be given a high focus by the SAMHS and the SAHC and become part of a larger telemedicine network. (7)
5. A higher level of clinical involvement in telepsychiatry be encouraged by the SAMHS, to ensure that sufficient medical practitioners are influencing policy and operational procedures. (7)
Secondary Recommendations
It is recommended that
- The SAMHS evaluate the use of desktop videoconferencing units, possibly one in a general practitioner location, one in a mental health team’s workplace, one with the sole country based psychiatrist and one at a metropolitan hospital. (7)
7. Induction and advanced training packages be developed, documented and implemented for all users, including psychiatrists. The induction and training packages be based on the concept that users can progressively develop more sophisticated levels of usage. (4)
8. SAMHS continue to pursue the issue of private psychiatrists receiving remuneration from the Medicare Benefits Schedule for the use of telepsychiatry. (5)
9. Legal and ethical issues related to the provision of clinical consultations on the telemedicine medium be investigated. (5)
10. Mental health teams at those country hospitals equipped with telepsychiatry facilities be encouraged to develop peer group dialogue and staff development activities, using the telepsychiatry facilities. (5)
11. Promotion and marketing of the facilities to more conservative thinkers, to general practitioners and to a wider range of psychiatrists be undertaken. (7)
12. Promotional brochures and other literature and a videotape on the project be developed and distributed. (7)
13. The existing network management publication be extended to include full accounts of the policy, procedures, methodology and training guidelines.
14. A fault log be kept, to assist in the clear delineation of the most frequent cause of problems and to aid in removing these causes and support staff be inducted on how to respond.
15. Marketing information about the project make clear that the videoconferencing facilities are available to all health related personnel.
16. Evaluation of user and client/patient needs, expectations and criticism of the telepsychiatry system be maintained in the second and third years of operation.
17. Statistics be kept of the number of times telepsychiatry enables a possible transfer of a country patient to a city hospital, to assist in cost benefit analyses of the medium.
18. Collaborative research be conducted with other telepsychiatry projects in Australia, such as the present one in Bendigo, Victoria
19. Improved service from the supplier of multipoint conferencing be negotiated.
20. Once the above recommendations have been acted upon, a separate consultancy be dedicated to defining, packaging and promoting the services in telepsychiatry that the SAMHS could provide to interstate and overseas organisations.
Conclusion
The audience for this report was the Telemedicine Steering Committee and it was deliberately written in a ‘warts and all’ fashion. However, readers should note that the 1994 pilot uses of the telepsychiatry network were generally very successful and encouraging and no more could have been done by the Steering Committee or the project co-ordinator and his team. The SAMHS should have every confidence that telepsychiatry can be an effective medium.